Thyroid disorders are among the most common medical conditions but are often misunderstood. Two primary conditions affecting the thyroid gland are hyperthyroidism and hypothyroidism. While both are related to thyroid function, they have different implications and require distinct approaches to treatment. In this blog, we will take a closer look at the thyroid gland and how these conditions can affect thyroid function.
What is the Thyroid Gland?
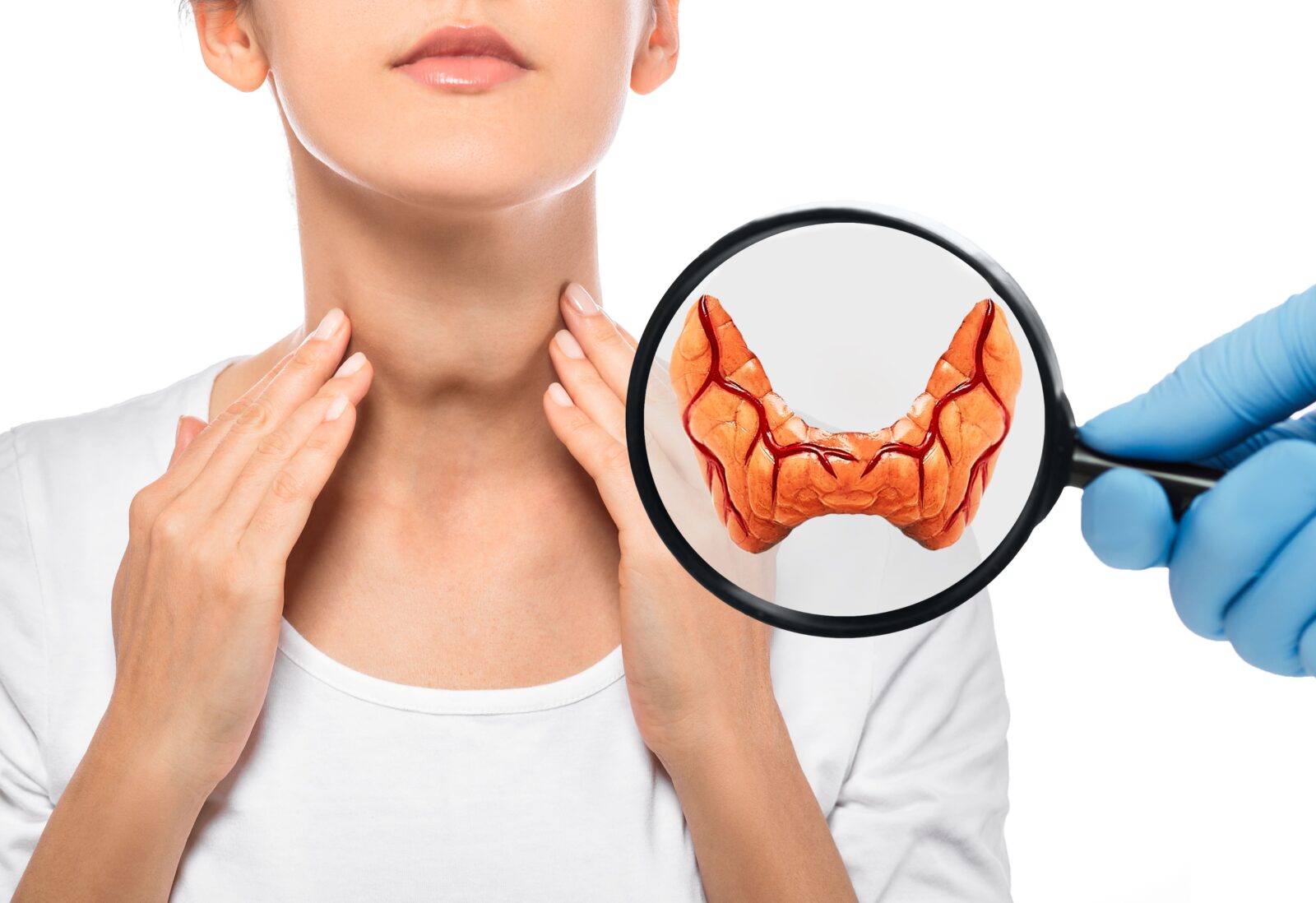
Before diving into the specifics of hyperthyroidism and hypothyroidism, it’s important to understand what the thyroid does. This small, butterfly-shaped gland in your neck produces hormones that regulate metabolism, which is how your body uses energy. These hormones impact your heart rate, body temperature, and even your weight.
Hyperthyroidism: The Overactive Thyroid
Hyperthyroidism occurs when the thyroid gland is overactive and produces too much thyroid hormone. This condition speeds up your body’s metabolism. The most common cause of hyperthyroidism is Graves’ disease, an autoimmune disorder. Other causes include thyroid nodules or inflammation of the thyroid gland. Symptoms of hyperthyroidism can include:
- Weight loss
- Rapid heartbeat
- Increased appetite
- Sweating
- Nervousness
- Restlessness
- Tremors
- Anxiety
- Difficulty sleeping.
Hypothyroidism: The Underactive Thyroid
In contrast, hypothyroidism happens when the thyroid gland is underactive and doesn’t produce enough thyroid hormone. This leads to a slowdown in metabolism. The most common cause is Hashimoto’s thyroiditis, an autoimmune condition. It can also result from thyroid surgery, certain medications, or radiation therapy. Hypothyroidism can cause symptoms such as:
- Fatigue
- Weight gain
- Slow heart rate
- Feeling of being cold
- Dry skin
- Hair loss
- Constipation
- Depression
- Memory problems
Diagnosing and Treating Thyroid Disorders
Ear, Nose, and Throat (ENT) specialists, also known as otolaryngologists, play a significant role in the diagnosis and treatment of thyroid disorders. Here’s how they typically approach these conditions:
Diagnosis
- Clinical Evaluation: The process often begins with a thorough clinical evaluation, including a detailed medical history and a physical examination. The ENT specialist will look for symptoms such as a swollen neck, difficulty swallowing, changes in voice, and other throat-related issues.
- Neck Palpation: The ENT doctor will palpate, or physically examine, the neck to feel for any abnormalities in the thyroid gland, such as enlargement (goiter) or nodules.
- Ultrasound: Ultrasound imaging is a key diagnostic tool used by ENTs. It helps in visualizing the thyroid gland and identifying nodules, cysts, or other structural abnormalities.
- Blood Tests: While ENTs don’t typically conduct blood tests themselves, they may refer patients for blood tests to measure levels of thyroid hormones (T3 and T4) and Thyroid Stimulating Hormone (TSH). These tests are crucial in confirming hyperthyroidism or hypothyroidism.
- Fine Needle Aspiration Biopsy (FNAB): If a nodule is detected, an ENT specialist might perform or refer for a FNAB. This procedure involves extracting a small tissue sample from the thyroid nodule to be examined for cancerous cells.
Treatment
The treatment approach depends on whether the patient has hyperthyroidism or hypothyroidism and the underlying cause of the disorder.
- Medication: For hyperthyroidism, ENTs may prescribe or refer for prescription of antithyroid medications to reduce thyroid hormone production. In hypothyroidism, hormone replacement therapy, usually in the form of synthetic thyroxine, is the standard treatment.
- Radioactive Iodine Therapy: This treatment is often used for hyperthyroidism, particularly in cases of Graves’ disease. It involves oral administration of radioactive iodine to shrink the thyroid gland.
- Surgery: In some cases, particularly when there’s a large goiter, nodules, or suspected cancer, surgery may be necessary. ENT specialists can perform thyroidectomies, which involve partial or total removal of the thyroid gland.
- Postoperative Care: Post-surgical care is crucial, especially in monitoring calcium levels and ensuring that patients who have had their thyroid completely removed start on hormone replacement therapy.
- Long-term Monitoring: Whether treated with medication, surgery, or radioactive iodine, patients with thyroid disorders usually require long-term monitoring. This involves regular check-ups and blood tests to ensure that hormone levels remain balanced and to adjust treatment as necessary.
- Referral to Endocrinologists: For complex cases, ENT specialists may work closely with endocrinologists, who specialize in hormone-related disorders, to provide comprehensive care.
Conclusion
While hyperthyroidism and hypothyroidism are both thyroid-related conditions, they have opposite effects on the body. Understanding these differences is key to recognizing symptoms, seeking appropriate treatment, and managing your health effectively. If you suspect you have a thyroid disorder, consult your healthcare provider for a proper diagnosis and treatment plan.