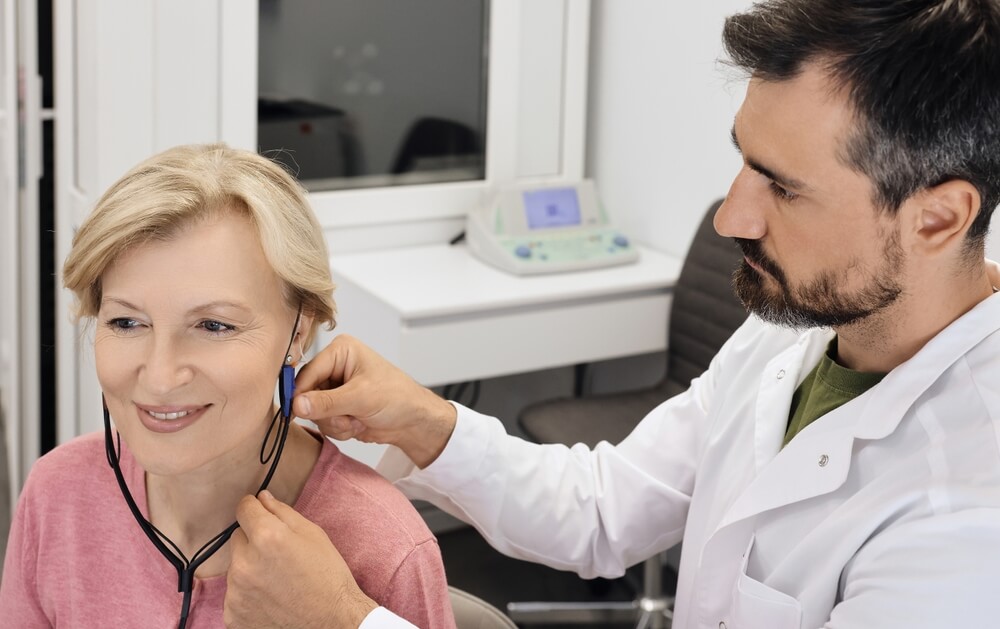
Many people consider scheduling a hearing test but delay making the appointment because they are unsure what the process involves. Hearing evaluations are straightforward, noninvasive, and designed to give a clear picture of how well the ears detect and process sound. Understanding what happens during the appointment can make the experience feel far more comfortable and predictable.
A comprehensive hearing test evaluates several aspects of hearing, including the ability to detect tones, understand speech, and assess how different parts of the ear function together. These tests help audiologists identify hearing changes and determine whether additional evaluation may be needed. Anne Arundel ENT & Facial Plastic Surgery serves patients in Annapolis and Severna Park who want to better understand hearing health and the role audiology testing plays in evaluating changes in hearing ability.
Why Hearing Tests Are Important
Hearing plays a critical role in communication, safety, and daily interaction with the world. When hearing begins to change, the effects may appear gradually. Conversations may seem harder to follow, especially in noisy environments, or certain voices may sound muffled or unclear.
Because hearing loss often develops slowly, many people do not immediately recognize the change. A comprehensive hearing evaluation helps identify subtle shifts in hearing ability before they become more noticeable.
Hearing tests also help determine the type and degree of hearing changes present. Some hearing concerns originate in the outer or middle ear, while others involve the inner ear or auditory nerve. By evaluating each part of the auditory system, audiologists can better understand how sound is traveling through the ear.
Educational resources such as comprehensive audiology testing help explain how these evaluations measure hearing sensitivity and provide valuable insight into overall auditory health.
Step 1: Reviewing Hearing and Medical History
The first step in a comprehensive hearing test typically involves a conversation between the patient and the audiologist. This discussion helps the specialist understand the patient’s symptoms, lifestyle, and hearing concerns.
Patients may be asked questions about situations where hearing seems difficult. For example, the audiologist might ask whether conversations are harder to understand in background noise or whether television volume has gradually increased over time.
Medical history is also important. Previous ear infections, surgeries, medications, and exposure to loud noise may all influence hearing. The audiologist may also ask whether there is ringing in the ears (tinnitus) or a feeling of fullness in the ears.
Gathering this information helps guide the rest of the hearing evaluation and ensures that testing focuses on the patient’s specific concerns.
Step 2: Visual Examination of the Ear
Before measuring hearing ability, the audiologist performs a visual inspection of the ear canal and eardrum. This step is performed using a small handheld instrument called an otoscope.
The otoscope allows the audiologist to look inside the ear to check for anything that might interfere with sound transmission. For example, the examination may reveal earwax buildup, irritation in the ear canal, or signs of infection.
Even minor blockages can affect hearing test results. Identifying these issues early helps ensure the hearing evaluation accurately reflects how the auditory system is functioning.
Step 3: Pure-Tone Hearing Test
One of the most well-known parts of a hearing evaluation is the pure-tone hearing test. During this test, the patient wears headphones while sitting in a quiet, sound-controlled room.
The audiologist plays a series of tones at different pitches and volumes. Each time the patient hears a tone, they indicate it by pressing a button or raising their hand.
This test measures the softest sounds a person can detect at various frequencies. The results are recorded on a chart called an audiogram, which provides a visual representation of hearing ability across a range of pitches.
The audiogram helps audiologists determine whether hearing changes affect low-frequency sounds, high-frequency sounds, or both.
Step 4: Bone Conduction Testing
Bone conduction testing is often performed alongside the pure-tone hearing test. Instead of headphones, a small device is placed behind the ear on the mastoid bone.
This device sends gentle vibrations directly to the inner ear, bypassing the outer and middle ear. By comparing the results of bone conduction testing with standard air conduction testing, the audiologist can determine where hearing changes may be occurring.
For example, this comparison helps distinguish between hearing loss caused by issues in the outer or middle ear and hearing loss related to the inner ear or auditory nerve.
Step 5: Speech Recognition Testing
Hearing involves more than detecting tones. Understanding speech is one of the most important aspects of everyday listening.
Speech recognition testing evaluates how clearly a person understands spoken words. During this portion of the exam, the patient listens to recorded words or phrases through headphones and repeats what they hear.
These tests help determine how well the brain processes speech signals. Even when tones are heard clearly, some individuals may still have difficulty understanding words, particularly in noisy environments.
Speech testing provides valuable insight into real-world communication challenges.
Step 6: Middle Ear Function Testing
Another important part of a comprehensive hearing test involves evaluating the middle ear. One of the most common tests used for this purpose is called tympanometry.
During tympanometry, a small probe is placed in the ear canal. The device changes air pressure slightly while measuring how the eardrum responds.
This test helps detect conditions such as fluid behind the eardrum, middle ear infections, or problems with the movement of the eardrum.
Because the middle ear plays an important role in transmitting sound vibrations, evaluating this area helps provide a complete picture of hearing function.
Step 7: Reviewing the Results
Once testing is complete, the audiologist reviews the results with the patient. The audiogram and other measurements provide detailed information about hearing sensitivity and speech understanding.
The audiologist explains what the results mean and how hearing compares to typical hearing levels. If hearing changes are present, the evaluation helps identify the type and degree of hearing loss.
This discussion gives patients a clearer understanding of their hearing health and how different parts of the auditory system are functioning.
When Hearing Testing Is Recommended
Hearing evaluations may be helpful in several situations. Many adults schedule hearing tests after noticing changes in their ability to follow conversations or understand speech clearly.
Testing may also be recommended when symptoms such as ringing in the ears, ear pressure, or sudden hearing changes occur.
In addition, individuals who work in loud environments or have a history of noise exposure may benefit from periodic hearing monitoring.
Regular hearing evaluations help track changes in hearing ability over time.
Understanding the Hearing Test Experience
For many people, the idea of a hearing test can feel unfamiliar. In reality, the process is simple, painless, and designed to gather valuable information about how the ears and brain work together to interpret sound.
A comprehensive hearing evaluation examines multiple aspects of hearing, including tone detection, speech understanding, and middle ear function. Each part of the test contributes to a clearer understanding of auditory health.
Anne Arundel ENT & Facial Plastic Surgery serves patients in Annapolis and Severna Park who want to better understand what happens during a comprehensive hearing test and how audiology evaluations help identify changes in hearing ability.
Sources
Gelfand, S. (2016). Essentials of Audiology. Thieme Medical Publishers.
Wilson, B., & McArdle, R. (2013). Speech signals used to evaluate functional status of the auditory system. Journal of Rehabilitation Research & Development.
Gates, G., & Mills, J. (2005). Presbycusis. Lancet.